July 12, 2018
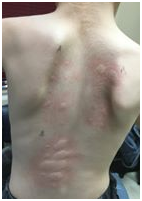 It was a moment that changed my life forever and my trust in the medical profession, a moment of such clarity and insight that I still feel it was divine led. It changed who I am, it transformed me from a sweet, trusting, happy mom to the questioning mom, the mom who thinks, the mom who asks before she acts.
It was a moment that changed my life forever and my trust in the medical profession, a moment of such clarity and insight that I still feel it was divine led. It changed who I am, it transformed me from a sweet, trusting, happy mom to the questioning mom, the mom who thinks, the mom who asks before she acts.
I had been such a diligent allergy mom—taking my daughter, who has a life-threatening peanut allergy, in for her regular skin prick tests. I wanted to know, I needed to be sure, what precisely is she allergic to? Was she truly allergic to peanuts (which I had observed with my own eyes when she was two years old)? I had followed the recommendations to the letter and had waited to introduce peanut butter. Upon one smear of that peanut butter, her mouth was instantly covered in large hives; a dramatic drop in blood pressure followed. And what about tree nuts? What about shellfish, dairy, soya? If one food had the potential to kill her, what about all the other potentially allergenic foods? The appointment with the pediatric allergist could not come soon enough.
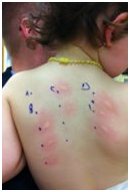 Allergy parents are all too familiar with the skin prick test—it is the go-to test for allergists to help figure out what their patients may be allergic to. A solution of the diluted allergen is placed on the skin, and a device is used to gently poke the solution into the body. If welts appear, that is a good sign that the patient may have an allergy. The welts can be big or small—the larger the welt, the more severe the allergy.
Allergy parents are all too familiar with the skin prick test—it is the go-to test for allergists to help figure out what their patients may be allergic to. A solution of the diluted allergen is placed on the skin, and a device is used to gently poke the solution into the body. If welts appear, that is a good sign that the patient may have an allergy. The welts can be big or small—the larger the welt, the more severe the allergy.
And so for nearly five years, I had diligently followed-up with the allergist, eager to make sure my allergy child was safe and eager to see if she had outgrown her peanut allergy. Her first skin prick test had shown a fairly mild reaction to peanuts, and the allergist was confident she would even outgrow the allergy. Of course, we also tested for every known tree nut. Thankfully, she was negative to all tree nuts at that first appointment. Still, being the conscientious allergy parent that I am, I never allowed my child to have tree nuts—I was too scared.
Every couple of years I found myself in the allergist’s office, testing once again for tree nuts—could she eat them? Could she not? There never was a definitive answer from the allergists, but they were helpful and kind, and we always tested for the tree nuts: pistachio, almond, brazil nut, you name it. Every time her allergies to tree nuts worsened, every time we added a new tree nut allergy to the list. The allergist was perplexed—he had been certain she was going to outgrow her peanut allergy, why was it worsening? And, again, keep in mind she started with no allergies to tree nuts. And we never, ever had tree nuts in our home, ever. And so, it suddenly crossed my mind—she had never eaten a tree nut. There never was really an opportunity for her to be exposed to tree nuts, the only place was in the allergist’s office through the skin prick test. Could it be? Could it be that the skin prick test was contributing to her allergies? And, could her peanut allergy have grown worse through the continual exposure to peanut only in the allergist’s office? I needed to know.
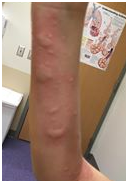 I went home and immediately spoke to a friend who is a brilliant biochemist from one of the best universities in Canada. “Could the skin prick test be causing and worsening my child’s allergies?” I inquired.
I went home and immediately spoke to a friend who is a brilliant biochemist from one of the best universities in Canada. “Could the skin prick test be causing and worsening my child’s allergies?” I inquired.
“Of course,” she said with confidence. “Isn’t that how we used to vaccinate people against smallpox? They used to employ a lancet to gently scrape the skin and place the smallpox antigen into the skin. And, every scientist knows this basic rule: Blood + antigen = antibody. This is the same for food protein and blood as well.”
(Allergy parents will tell you that sometimes there are a few drops of blood with the skin prick test—but also, the food protein solution can seep or soak into the bloodstream, similar to hormone patches.) My biochemist friend also told me how she never allowed her own children to have skin prick tests and that avoiding the potential allergen might just have the advantage of helping the immune system forget about the allergy. (Imagine the skin prick test as being a type of “booster shot” for the child’s allergy.)
I then went on to read anything I could get my hands on in terms of how the immune system worked. I read all the pioneers in immunology, like Dr. Charles Richet—he had won the Nobel prize for his experiments with antibodies and vaccination. He had learned that whatever was injected into the body (and thus could bypass the normal routes of entry to the bloodstream) resulted in the creation of antibodies, and this could also apply to food. It worked like magic. (You can read his crystal clear discussion of his experiments with this principle in this Nobel prize acceptance speech.)
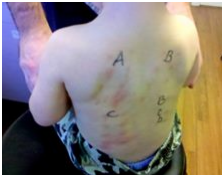 I also heard, through the grapevine, of a well-known allergist (who cannot be named here) who advised their patients to avoid skin prick testing altogether. And again, through the divine, I had a strange visit with our well-educated optometrist—their (I use the gender-neutral pronoun to preserve the anonymity of these doctors) child had a peanut allergy. They furtively whispered to me during an eye check-up for the children, “What do you think of the skin-prick test?”—they then went on to explain how their child had suffered an anaphylactic type event during skin testing. The insanity of it all became increasingly baffling—here we are in everyday life, as allergy parents, doing all we can to keep our children safe from their allergies, yet in the allergist’s office we invite them to put these allergens directly into our children’s system.
I also heard, through the grapevine, of a well-known allergist (who cannot be named here) who advised their patients to avoid skin prick testing altogether. And again, through the divine, I had a strange visit with our well-educated optometrist—their (I use the gender-neutral pronoun to preserve the anonymity of these doctors) child had a peanut allergy. They furtively whispered to me during an eye check-up for the children, “What do you think of the skin-prick test?”—they then went on to explain how their child had suffered an anaphylactic type event during skin testing. The insanity of it all became increasingly baffling—here we are in everyday life, as allergy parents, doing all we can to keep our children safe from their allergies, yet in the allergist’s office we invite them to put these allergens directly into our children’s system.
Then came the Dr. Lack study which suggests that children with eczema develop food allergies through exposure to peanut dust floating around their homes that creeps into their wounds. Again, the scientific principle remains: Protein (antigen) + blood = antibody. I remember excitedly writing to Dr. Lack; clearly he must see the connection between the skin prick test and his eczema study—it’s all so much the same. Should we not be using the precautionary principle and avoid skin prick testing given the risks? Silence.
Recently another study points towards baby wipes as also breaking down the skin barrier and allowing food proteins to soak into children’s bloodstreams. All these studies remind us of the basic biological principle—don’t mess with Mother Nature’s natural barriers, especially when it comes to food. Again, remember how the body processes food—digestion begins in the mouth where saliva begins to break down food protein, then the stomach where stomach acid continues this process, then the long journey through the intestines—but again, undigested food proteins do not belong in the bloodstream, they belong in the digestive tract.
Yet, in the allergist’s office it seems there is some magic fairy dust that appears to circumvent this biological fact. In the allergist’s office, it seems we can violate the skin barrier and suffer no consequence: we can do this in name of medical science and safety and security and the need to know, the need to be sure. It needs to be pointed out that there is a blood test that is reliable for food-allergy testing, there are other avenues to help us figure out what our children are allergic to.
In my journey for answers, for credible science, I found one brave female immunologist who was willing to speak out. Dr. Janice Joneja is a courageous doctor with impressive credentials—a Ph.D. in microbiology and immunology. She is also a pioneer in the field of food allergy due to her own experience with her son who struggled with food allergy growing up.
Through the years she would hear stories from moms who found, just like me, that their children were developing allergies to foods they had only been exposed to through the skin prick test. And, unlike other allergists, when they told her this, she listened. Not only that, she spoke out—at great risk to her own career. After my own life-defining moment with the skin prick test, I remember suggesting at a follow-up appointment with a male allergist that I believed the skin-prick test was risky. I said to him, “I have observed new allergies developing in my child, and I believe the skin prick test may be to blame. There is another immunologist who also feels that the skin prick test needs further investigation, Dr. Janice Joneja.” This allergist sneered at me, and condescendingly dismissed my concerns, and he said, “As for Dr. Joneja, she is highly, highly controversial.” As so many of us thinking moms know, even in this era of feminism, of female empowerment, asking questions of the medical establishment is forever risky.
But Dr. Joneja has not given up caring about our children. When I contacted her, she implored me to go into allergy groups and share the risks of skin prick testing. So, today, with her blessing and encouragement, I am sharing with the TMR community a reprint of Dr. Joneja’s most recent exploration of skin prick testing (this too comes with the approval of the kind editor of the foodsmatter site).
Dr. Joneja is incredibly well-educated and has dedicated her life to understanding allergy: Again, she holds a Ph.D. in medical microbiology and immunology. She has held faculty positions at several universities, including the University of British Columbia (Vancouver, BC, Canada), and has taught at universities and colleges throughout Canada, the U.S.A., the U.K. and other English-speaking countries. She was a registered dietitian (RD) in British Columbia for 27 years and a member of the Academy of Nutrition and Dietetics in the U.S.A. For 13 years she was head of the Allergy Nutrition Clinic at the Vancouver Hospital and Health Science Centre.
Dr. Joneja is the author of 10 books and dietetic practice manuals on immunology and food allergy, a textbook on Irritable Bowel Syndrome, and a number of distance education courses. Her work has been published in peer-reviewed scientific and medical journals as well as in popular magazines. She is a respected lecturer at universities, colleges and hospitals internationally and regularly appears on television, radio call-in shows, and online webinars as an expert in her field.
She is president of Vickerstaff Health Services Inc, a practice that provides individual counseling for people suffering from all aspects of adverse reactions to food, and resources for the professionals and caregivers who support them.
Allergy moms and dads, I understand your anxiety, your desire to do the right thing, the urge to keep your children safe. So I present to you the most up-to-the-minute scientific evidence to help you decide for yourself whether or not the skin prick test is worth the risk. I also look forward to hearing your stories: Did you notice a worsening of your child’s allergies after the skin prick test? Did your child develop new allergies after skin prick testing? Did your child have an anaphylactic event during this test?
Remember, medicine is always changing its opinion on what is safe and unsafe—at one time smoking was considered safe, at one time they x-rayed pregnant women, and at one time doctor’s delivered babies with filthy hands.
It is your child: Be brave. Ask questions. Be kind, but not too trusting.
With love and encouragement,
~ The Allergy Whisperer
For more by The Allergy Whisperer, click here.
And with no further ado, I present Dr. Joneja, reprinted from foodsmatter:
Skin Prick Testing as a Cause of Food Allergy? |
| Could skin prick tests cause the allergies that they are designed to diagnose? Dr Janice Joneja believes that they could.
See here for comment from allergist Dr Adam Fox. |
| The accurate diagnosis of food allergy and food intolerance is fraught with difficulties. No single test can definitively identify the food components responsible for the clinical expression of an immunological or non-immunological reaction to a food. In the end, elimination and challenge must be undertaken to determine the precise role of a food component in triggering symptoms.
(Image of skin prick test being performed courtesy of the Medical Journal of Australia.) It is well known that many agents can be effectively delivered to the body via the skin. Hormones, vaccines, antitoxins and proteins are efficiently introduced into the body via this route, circumventing the digestive tract and powerfully targeting the effector system for which they are designed. There is no reason to suppose that allergens delivered through the skin by absorption (in a patch), by injection (intradermally) or by pricking or scratching, should not induce allergen-specific IgE in a similar manner. Tolerance versus sensitisation; the gut versus the skinOur immune system is designed to protect the body from any foreign substance that enters. In this way we are protected from invading micro-organisms, toxins and other noxious agents that pose a threat to our health and survival. Of course, all food is entirely foreign to the body, and as such should logically be rejected by the immune system. So, how and why does this not occur? It is all due to a process known as “oral tolerance”, which distinguishes between “foreign and a threat” and “foreign but safe”. Oral tolerance is achieved by a very complex series of reactions of immune cells lining the gastrointestinal (digestive) tract, directed by T-cell lymphocytes. The molecules in the intestinal contents from food, beverages and other ingested material are sampled, analysed and responded to by the immune cells. If safe, the material is then allowed into the body. When the same material is ingested on future occasions, it is recognised as safe and no adverse immunological response occurs. However, if tolerance to the substance does not occur, the immune system will reject it; in the case of food, this response results in allergy. When the food material enters the body via a route other than the digestive tract, it is assumed to be a threat unless previous tolerance has been established via the oral route. Exposure to food antigens through the skin is more likely to lead to allergy compared to early oral consumption, which is more likely to lead to tolerance. I have provided details about the processes of immunological tolerance and sensitisation in my books and articles on food allergy, and a good review of the topic can be found in reference Izadi 2015 below. Allergen exposure via the skin
New research confirms this route to sensitisationA recent research study at Northwestern University in Chicago demonstrated that in genetically predisposed mice, exposure to food and environmental allergens through the skin led to the development of allergic markers such as inflammation, inflammatory mediators and anaphylactic reactions after the mice were fed the allergenic food (Walker et al 2018). Interestingly, mice of allergic mothers were more likely to develop reactions to lower sensitising doses of the allergenic food. Following publication of this research, the idea that human babies could be similarly predisposed to be at risk of allergic sensitisation was suggested. An article in the popular press warned parents that using baby wipes could initiate food allergy by facilitating the passage of the food through the skin (Bodkin 2018). Scratch and prick tests Dr. Janice Joneja It is ironic that the authors should suggest baby wipes as a means of facilitating the introduction of the allergenic food to the immune system, while ignoring the most obvious mechanism of intradermal exposure, namely scratch and prick tests commonly used in an effort to diagnose allergy to a specific food. In such tests, allergen extracts are placed on the skin, which is scarified with a lancet or pricked with a needle, to ensure that the allergen encounters immune cells beneath the surface. In intradermal testing, the allergen is actually injected into the skin, thus ensuring an even greater exposure to the immune system. All of these tests are incredibly efficient methods of delivering the allergen to the immune cells, which are more than ready to respond, with rapid development of food-specific IgE that, in predisposed children can, and will, lead to food allergy, and in severe cases, anaphylaxis—as demonstrated by the 2018 article mentioned above. Many allergists will not skin test their atopic patients with highly allergenic foods, such as peanuts and nuts, because they are aware that antigen delivered via this route can trigger an anaphylactic reaction. It is only logical to assume that primary sensitisation can occur by this route. After all, vaccination using antigen delivered on skin patches is proving very effective (Partidos et al 2002). Have allergies been caused by these diagnostic methods?I often wonder how many innocent children and their unwitting families have been sentenced to a life-time of dealing with the miseries of allergies as a result of the tests so commonly used in diagnosis. I have actively discouraged my patients, especially atopic children, from having skin tests performed because of the risk of inducing IgE via this route. In good conscience I could never condone any action that might result, in an extreme case, in a life-threatening anaphylactic reaction. Even milder reactions can result in a life-time of misery. Until I see well-conducted scientific research that proves that there is no possibility of immunological sensitisation through this route, I shall continue to dissuade my patients from undergoing this method of allergy testing. Alternative methods diagnostic proceduresThere are alternative in vitro methods for detecting allergen-specific IgE; RAST, FAST and ELISA tests have the potential for providing information that in most cases is as useful as any skin test. The cost and need for laboratory facilities might limit their use for the present, but refinement of the technique should make them more economical and universally available in the near future. The newer techniques of component resolved diagnosis (CRD) which are currently being developed may prove to be a concise method for allergen identification in the future. Hopefully, awareness by clinicians of the potential for primary sensitisation to allergens through the skin will stimulate the speedy development of more specific in vitro tests, and discontinuance of the risky practice of skin testing in all its forms. References Blyth T, Lack G. Are we generating peanut allergy? Asthma J 2002;7:120-122 Bodkin, Henry. Baby wet wipes ’cause food allergy’, new study warns. Daily Telegraph April 7 2018 Izadi N, Luu M, Ong PY, Tam JS. The role of skin barrier in the pathogenesis of food allergy. Children 2015;2:382-402 Khakoo A, Lack G. Preventing food allergy. Current Allergy and Asthma Reports 2004 Jan;4(1):36-42 Lack G, Fox D, Northstone K, Golding J. Factors associated with the development of peanut allergy in childhood. New Eng J Med 2003;348:977-985 Matsuoko H, Maki N, Yoshida S, Arai M, Wang J, Oikawa Y, Ikeda T, Hirota Partidos CD, Beignon AS, Brown F, Kramer E, Briand JP, Muller S. Applying peptide antigens onto bare skin: induction of humoral and cellular immune responses and potential for vaccination. J Control Release 2002 Dec 13;85(1-3):27-34 Radhakrishna N, Prickett S, Phan T, Rolland JM, Puy R, O’Hehir RE. Anaphylaxis to oats after cutaneous sensitization by oatmeal in skin products used for the treatment of atopic dermatitis. J Allergy Clin Immunol Pract. 2016 Jan-Feb;4(1):152-3. Saloga J, Knop J. Does sensitization through the skin occur? Allergy 2000;55:<905-909 Voskamp AL, Zubrinich CM, Abramovitch JB, Rolland JM, O’Hehir RE. Goat’s cheese anaphylaxis after cutaneous sensitization by moisturizer that contained goat’s milk. J Allergy Clin Immunol Pract 2014 Sep-Oct; 2(5):629-30 Walker M, Green J, Ferrie R, Queener A, Kaplan MH, Cook-Mills JM. Mechanism for initiation of food allergy: Dependence on skin barrier mutations and environmental allergen co-stimulation. J Allergy Clin Immunol 2018 Feb 15;[Epub ahead of print] April 2018 |







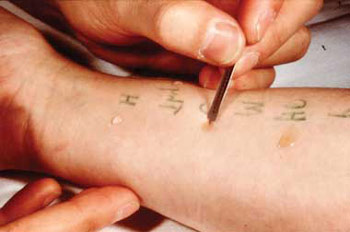 Although skin testing is still the only in vivo test that is universally employed in clinical practice, its potential hazards have been greatly underestimated.
Although skin testing is still the only in vivo test that is universally employed in clinical practice, its potential hazards have been greatly underestimated.









hello can you send me the standard protocol for the skin prick testing
Bringing this study, published last month, to your attention in light of your article.
How much can we win if we were to get ahold of the list of food adjuvents added and bet on subsequent rise in allergies to foods containing these ingredients?
https://www.ncbi.nlm.nih.gov/pubmed/31554190
Vaccines (Basel). 2019 Sep 24;7(4). pii: E127. doi: 10.3390/vaccines7040127.
Food Additives as Novel Influenza Vaccine Adjuvants.
Abstract
Influenza is a major threat to public health. Vaccination is an effective strategy to control influenza; however, the current inactivated influenza vaccine has mild immunogenicity and exhibits suboptimal efficacy in clinical use. Vaccine efficacy can be improved by the addition of adjuvants, but few adjuvants have been approved for human use. To explore novel and effective adjuvants for influenza vaccines, here we screened 145 compounds from food additives approved in Japan. Of these 145 candidates, we identified 41 compounds that enhanced the efficacy of the split influenza hemagglutinin (HA) vaccine against lethal virus challenge in a mouse model. These 41 compounds included 18 novel adjuvant candidates and 15 compounds with previously reported adjuvant effects for other antigens but not for the influenza vaccine. Our results are of value to the development of novel and effective adjuvanted influenza or other vaccines for human use.
Thank you for this, I will take a look right now.
Thanks for helping me understand that the process is only going to make you feel a gentle poke on your skin with a diluted solution. I just needed to know about this since I need to find out why my son got rashes this evening. He is too young which is why I need to know if he will be alright. I have a feeling that he might be allergic to the shrimp that we served for dinner, but we need to be sure.
How did it go when you went to the doctor? Allergists (doctors) can seem so caring and trustworthy. It can be hard to say no to the skin prick test–it also gives the promise of instant information, which is very tempting when we want to keep our children safe.
I have severe anaphylaxis reactions starting w several bites from a yellowjacket that flew in car window into my shirt. Then my peanu,fish, shellfish allergy became worse and airborn. And a long list of chemicals and other allergens began..my immune system has spun to hyper sensitive that If someone else ate peanuts or shook my hand after even though I weardlivrs and 2 masks. I have had anaphylactic reactions and it is worse when I travel, been treated in ER and urgent care clinics in 5 states. I tried the blood test by two well known specialists for all the food and enbirinme talk allergies and they came out with false negatives..baffling the doctirs..i was told by 4 different allergy clinics and 3 nurses and 1 expert doctor at a university it would be unwise to do a skin prick test. They said the only course is avoidance yet each anaphylaxis event escalated me to death. But all allergist refuse to treat me without the skin test. Yet the skin test could kill me. Yet their only solution is a skin test in a hospital so if I begin to die they can take heroic measures and bag me put hole in trachea etc..
Yet my allergist says without skin test by law they can not legally treat me with shots because they have no way to know how much medicine to put in the shots. So is a catch 22 isn’t it. If I don’t have skin tests done I
can’t get treated they say. If I do nothing my allergies will eventually escalate anyhow to death..as I already had 11 anaphylaxis reactions to various allerhebs. Appate fly the blood tests only can test for 1 protein allergen marker and any given allergen may have 300.. so blood tests not as accurate as skin tests..yet read skin rests are 50% accurate anyhow.. so they sending me to another specialist in hopes to test me in hospital, but reading how this test of several allergens put direct into blood stream could escalate my allergies further..i am at a loss if that is worth the risk since just one allergen on list they test for could cause anaphylaxis which means several allergens put directly into blood stream and multiple anaphylaxis reactions.
They say is why they would test in a hospital setting so if I go I to anaphylaxis shock which I know I alrewady have from just one allergen on the list..they told me that If I don’t have the skin rests I coukd die anyhow because my system already so hypersensitive..so anyone have any knowledge about skin tests on a person who is already anaphlaxis..would love to hear more info..doing nothing could hasten death But doing the skin tests could hasten it also..the blood tests had twice at reputable labs and they showed false negatives..showed not one thing i was allergic to when I super allergic to most items on list and been treated for anaphlaxis fpr it in 5 states. docs are baffled and shocked tests showed nothing ..but this doc said she saw hard cases like this b4 that blood tests not shoe accurate results is whtbthey prefer skin testing more accurate.
Recently sent for breathing tests for
Asthma each an 1 hour long..when test administrators saw how sensitized I am they thankfully said they not recommend I go thru one of the tests bcuz involved injecting my lungs w a poison and creating a severe asthma attack..i was so grateful they told me..and told my doctor I refuse that test we already know I have asthma no need to create more problems like life threatening asthma attacks on purpose is there??? Why doctor would order that test and put me thru such misery when she knew how severe and life threatening my attacks were I really can’t u understand that is in line with oath to do no harm..is it??
SO can encourage ALL to not be intimidated but for the courage and need to do yiyr researvh, and ask tons of questions..get other opinions..big need to weigh risk/benefit ratio for any test or medicine or therapy u doctor prescribes..not rush into any kind of treatment without researching it.
be an informed patient as u have the basic human right to refuse any treatment, medicine, or test you not agree with and u can carry a medical directive or durable power of attorney or living will on u once u know what treatments u will not accept so in case u can’t speak for yourself u have a way to inform medical ER care staff
Express your wishes which they must respect by law is basic human right to determine what is done by medical staff and give medical instructions what u will accept being done to your body.
…………..
For example blood transfusions used to be old gold standard of care..but was developed and considered fairly new protocol during world wars..yet since then over 60 safer and more cost effective alternatives have been developed and bloodless medicine around the world is now the NEW GOLD standard of care.
For more info..Google Kriever inquiry red cross blood scandal in Canada where they had no choice but to shut down the entire country red cross system because the socialized gov. medical system knowingly gave tainted blood to thousands who later developed hepatitis C aids/hub and s boat of other diseases.the quieriex the anestitists (Who administer blood transfusions) and 60% of them said they would not personally take a blood transfusion. I met a lady who was in a car accident was given 75 transfusions w tainted blood and she had wished she knew ahead about carrying a spa durable power of attorney with her wishes to habe only Bloodless medicine and refuse blood transfusiina. Her and her husband are now dying of hepatitis C she got from.red cross tainted blood supply and Canada gov.gave her a legal settlement for but she passed to her husband and her kids will soon lose both parents.
Bloodless medicine alternatives have saved her life had she known about it.
At least 60 bloodless alternatives that do not have those life threatening risks, or worry of blood tainted pathogens unscreened for like blood transfusions have.
All types of surgery including trauma cases have Ben performed successfully without blood..back.in the 1970s
Dr. Denton Cooley pioneered the first bloodless alternatives so people would not have same risks of developing infections as they would from unknown pathogens unable to be screened in blood transfusions.
Patients who choose bloodless medicine slternatives must discuss bloodless medicine alternatives ahead of surgeries etc.to make sure the hospital is up to date on and well equipped and prepared informed with these new gold standard of health care alternatives.. so they can ensure tgey choose an up to date medical facility with skilled staff who are updated on this new technique.
Often times patients may find their doctor refer u to a much more qualified expert specialist..a few friends of mine had triple bypass surgeries and when they informed doctorprior to surgery at initial consult that they wanted the new gold standard of bloodless medicine alternatives, instead of yhe old protocol transfusions the heart surgeon said I am just not that good, u need someone more precise ( in oyhlter words not as sloppybecause can’t lose one drop of blood)!
I will refer u to a better surgeon yhen me, and hospital equipped and specializing as a bloodless medicine hospital center. Because when your surgery isyhe new gold standard of care, using the over 60 bloodless alternatives habe to be chosen in advance, the surgeon has to be more precise in the amount of incision/cuts and careful not to lose any drops of blood during surgery so u will get even better medical care if u request that!
But U MUST prepare and consult to find a doctor abreast in bloodless medicine alternatives but is so worth the extra preparation and speedier recovery with less complications. My friend went home after only a few days versus a few weeks or more that other patients who had same surgery with old transfusions of blood protocol suffered infections and complications from, due to tge transfusions given during surgery.
SO is now gold standard of medicine to do bloodless surgery alternatives, and to be an informed patient..and this is example of why there is often other alternatives out there to various medical treatments out there that you have to research yourself. But is worth the better recovery and health results, and less life threatening risks for sure.
Keep on mind every treatment or medicine carries a risk or side effects you have to weigh that risk with the benefit.
P.S.
An excellentresource with accurste online library w various medical and other useful topics..website I found with also a section besides articles of videos for the doctors and patients on bloodless medicine I found is http://www.jw.org
Oh my goodness what a journey you have had. I’m so sorry for all you have been through. One doctor told me that allergists can bill directly for skin prick testing, that is why they like it so much. It’s an instant source of income. With the blood test the lab gets to bill. Sad truth. Very interesting about the bloodless medicine, so important to never stop asking questions.
“I’m sorry, John, but that response is hilarious. You have to look for financial factors when a SMALL number of people “say or promulgate something counter to the vast majority of other scientists”?”
I was referring to the groups of people who exploit sick/injured patients who are desperate for a cure, and will pay any amount of money out of hopelessness, but claim they are being hounded by the scientific community. Example – a friend of mine who was going to have his recently diagnosed esophageal cancer treated (to the tune of $50,000 up-front) at a clinic in Mexico where the main “therapy” was the long discredited Laetrile (he is doing quite well, now, with standard therapy), or those who have, say, a well-recognized, well-treated disease (diabetes, certain cancers, cardiovascular disease) and, eschewing traditional, well-researched, and standard treatment, fall prey to the mountebank, charlatan, and dangerous quack. Would you go to a chiropractor for treatment of a heart attack? Or an accupuncturist for treatment of a melanoma? Or a homeopath for treatment of multiple sclerosis? I know people who have done each of these behaviors, to their detriment.
It is important to recognize that here we are talking about a diagnostic test as opposed to a therapeutic procedure. At best, skin testing for food allergy has less than 50% accuracy rate, and all results need to be subsequently confirmed by elimination and challenge with the suspect food. Introducing foreign material through the skin in order to induce an immune response is acceptable when the procedure leads to protection, as is achieved with vaccines. It is not acceptable when the procedure has merely questionable diagnostic value and can lead to allergic sensitization in susceptible children. The only beneficiaries in the latter cases are the clinicians and their assistants who administer the tests and the rich and powerful drug companies who produce the allergen extracts and testing supplies.
Yes, it is a diagnostic test; I hope no one imagine it’s therapy. The false negative rate is essentially 0; it is quite sensitive (not sure where your less than 50% comes from). Do you really want people to undergo the expense of blood tests, which aren’t usually very specific?
Several practitioners have stated in print that skin tests in the diagnosis of food allergy are without merit and should be discontinued. For example, the late Dr. Keith Eaton found in his practice that skin prick testing for determining a patient’s allergenic foods had an accuracy of only 28% when confirmed by elimination and challenge. He writes, “It is therefore suggested that the use of skin prick tests in the diagnosis of ingestant responses to foods should be discontinued.” (Eaton 2004). Dr T.J.David, a noted British Paediatrician states in his book, “Food and Food Additive Intolerance in Childhood”, “Skin prick testing still has its enthusiasts. They tend to be based in the specialty of allergy, where there may be a perceived need to demonstrate “allergy expertise” or where the performance of tests is associated with a fee for service. Although skin-prick testing has a place in research studies, it is difficult to see a place for skin testing in the general diagnosis or management of allergy or intolerance to food or food additives” (David 1993 p 251).
With regard to false negative tests for foods being 0: This applies only to a few select, highly allergenic foods. It does not apply to all foods. The incidence of false positive tests for foods is at best only 50%. Do these statistics really justify the risks?
Concerned readers will find information regarding the value of skin prick tests (SPTs) in the diagnosis of food allergy in the following article:
Eigenmann, P. A. and Sampson, H. A. (1998), Interpreting skin prick tests in the evaluation of food allergy in children. Pediatric Allergy and Immunology, 9: 186-191
Important statements by the authors include,
“..the precision of STPs is limited by an apparent variability of sensitivity and specificity to different food antigens, and by the low positive predictive accuracies when used as a screening test in a general allergic population.” “Skin prick tests are a useful procedure for evaluating reactivity to egg, milk, peanut and wheat, but not to soy.”
I am certainly not doubting that some people have problems after allergy testing, but even assuming it has been definitively shown to be related, a large swath of people do benefit, and to regard a belief in it as anti-science is just ludicrous.
As with the link that many believe exists between (some) vaccinations and autism, it clearly doesn’t affect everyone who gets an immunization, and there is benefit to many. Why some develop autism is not yet determined (association doesn’t determine causality) and more research into the developing brains of those who develop spectrum diseases is needed, but it will come from science, not speculation.
The tinfoil comment was specifically in reference to Maurice Battle’s comments which were just so bizarre it seemed like he/she was participating in an alternative thought process; it wasn’t directed to anyone else, nor meant for anyone else. Unfortunately, the posting follows its own algorithm and wasn’t spaced accordingly. Sorry if anyone took umbrage.
A great deal HAS been determined as to why some develop autism, as is evident if you read The Environmental and Genetic Causes of Autism, as I have suggested to you multiple times.
I wrote “Why some develop autism”, implying (to me at least) that why others develop it has been established. I have read several essays on environmental and genetic causes of autism, and am sure that there are established factors. I am also willing to offer the opinion that vaccinations MAY trigger a confluence of events that leads to autism.
Ah, I see. The wording made it sound like you meant the “some” that DO develop autism. I understand your meaning now.
I appreciate you taking the time to write Mr. Collins. People presenting with allergy already have very sensitive immune systems. Thus, it probably takes a lot less to sensitize them than the average person. Think about how people develop allergies to bees and wasps for example. The bee stings the person, breaks the skin, and injects a bit of venom. The body responds with antibodies. The next time the person is stung an allergy may result. This doesn’t happen to everyone as so many of us have been stung and never develop an allergy. Now, I believe most medical professionals are aware of the precautionary principle, or at least still make the pledge “first do no harm.” Skin prick testing is of little benefit if your child ends up with anaphylaxis, has their body re-educated on an existing allergy, or develops new ones. Point being, there are other ways of testing, so why not leave this test in the dust? I’ve also heard, at least where I live, that allergists can bill in office for the skin prick test; however, blood tests are billed by the lab. So, you can see there is some financial interest in it for the allergist–the skin prick test is probably mostly how many of them spend their days. But again, thank you for clarifying your comments.
While I have no doubt that financial motivation may influenceSOME medical care, a large part of it may simply be inertia. Several cogent papers suggest that changing established behaviors in medical practice take up to 17 years to develop (for example, giving a low-dose aspirin in chest pain), so changing the practice of skin testing by skin prick rather than blood testing may be the same. Every test has its own sensitivity and specificity; virtually nothing in medicine is 100%, so if your physician has had experience and good results with an intervention, it might be difficult to change a style of practice.
Remember, hypersensitivity after skin prick testing is relatively uncommon, and alternative means of testing may miss some true positives. Like much else, there are trade offs.
regarding allergy tests (skin prick ones), yrs ago I suddenly developed a serious allergy to some local anesthetics. After that I had tests for several which the local dentist used, and showed up allergic or “suspicious” to all. For about fifteen or more yrs, any dental work was done without freezing. (I became a very good brusher). Eventually, I moved to another place, and the dentist sent me to allergist to see if they thought it worth testing again. That allergist (and several there after), insisted I bring ONLY one sample of dental anesthetic directly from my dentist’s office, and I be tested only on ONE, the one they actually used. They said that sometimes I may be ingredients besides the “freezing” which cause the allergy, and that dentists order from different sources, which may have differing incipient ingredients. Also was suggested I not “routinely” have these tests, as they stated (the allergist) that these tests can themselves initiate an allergy/more severe allergy. ====
of course there was the one allergist I went to who refused to test me as he said it was “ridiculous” as a person could not be allergic to this.
There are two types of anesthetics, esters and amides. Some people have a reaction to one, typically the amides, but not the other.
One way of determining is by the name. Amides typically have two “I”s in the name, such as Bupivocaine or Lidocaine (Xylocaine uses the Y like an I), while esters have only 1 I, such as Procaine or Marcaine.
Should you need anesthetics again, this may help you to avoid something that could cause problems (cocaine, originally and still occasionally used as a topical anesthetic, especially in Nasal surgery is another matter)
wow, what a story, sorry to hear about all those years of painful dental work–it’s nice to hear there are some awake allergists out there. . .
sigh…It is sad that when a group of folks are trying their best to share what has worked for them, and info they have worked hard to research, are harassed. Regarding the person making the tinfoil comments, one has to wonder what sadness is going on in tinfoil’s life, that he frequently feels the need to make nasty comments…
Yes, clearly we have many unexplained epidemics out there–in the absence of answers, is it not wise to question everything? and to look for answers?
There aren’t that many unknown or unrecognized epidemics, but there may be clusters of diseases that occur.
allergywhisperer ———————
absolutely…question everything. Think over everything. EVERYTHING . Sadly I have found that even experts who are well meaning, are often ill informed/ill educated.
I knew the anti-science fervor in this country was bad, but I had no idea how delusional some people can be. Really believe in flat Earth, age of the Earth under 7000 years, astrology?
Unfortunately, once people realize that their faith in their government agencies and their doctors to keep them safe is entirely unfounded (or was founded on some execrable “science”), some do react quite badly and assume that nothing “accepted” is the truth, especially if their brains are muddled by high levels of toxic metals. Fortunately, that is by no means the rule. Thankfully, completely rational people with integrity are engaged every day in questioning the “received wisdom” or doctors would still be going from cadavers to delivering babies without washing their hands and we would still think that saturated fat is responsible for the health problems that sugar causes.
Read and understand the science in Dr Joneja’s article. Anti-science would believe in the skin test!
As a general rule, when a very small number of people say or promulgate something, counter to the vast majority of other scientists, you have to look for financial factors.
I’m sorry, John, but that response is hilarious. You have to look for financial factors when a SMALL number of people “say or promulgate something counter to the vast majority of other scientists”? How about looking for the financial factors when a small number of people and corporations are CONTROLLING THE SCIENCE THAT IS BOTH PERFORMED AND PUBLISHED? THOSE are the “financial factors” that should be concerning you the most. Tobacco company science and oil company science is obviously corrupt to anyone who can think; it’s the science that is controlling the consensus that you should be paying attention to.
What else is in the allergy solution? A dr once told an audience at an autism conference that the allergy tests contain Thimerasol. Which backs up an earlier comment. Read the book about peanut allergy epidemic. Oh mr
Collins—-the tinfoil hat stage is over. We are on to the “vehmently oppose” and soon this will all obvious and accepted. Injecting toxins into anyone is always a bad idea. We are pointing out that we are using two-century old medical technology and you are riduculing US???
Thank you Carolyn, I will see if I can find out the precise ingredients in the solution. I will follow up.
Hello. Thank You for sharing Your story with us. My son is allergic to diary, eggs, tree nuts. Every six months we have a skin prick test recommended by his immunologist. The last time he had a severe reaction after he was injected by diary diluted solution, and the doctors gave him some drugs to recover for he was swollen in entire face. He showed a regression in diary allergy in the last years, and this last reaction was a total surprise and anxiety for us. Now I understand that may be the reason to this reaction is the skin prick test. But what is the alternative? How we will know that the allergy is gone when we do not do some tests to our children?
blood test
Hello Allergicson, I’ve heard many stories now of children having anaphylactic type reactions to skin prick testing. My own child had a similar type of anaphylactic reaction during skin prick testing as well. There is a very reliable blood test you can ask for that will help you monitor all those levels. I will also ask Dr. Joneja if she might hop on here and answer some of your questions. Also, keep in mind, the field of allergy is rather new. One key chemical player in allergy is histamine. Each time you do skin prick testing you flood the body with histamine–we want to be calming down histamine, not adding more histamine.
There are non-invasive blood tests available that do not involve introducing allergens into the body.
Thank you Allergy Whisperer. It is my hope that this outstanding article may help end this barbaric practice. When new to the allergy world a couple of decades ago, I remember an allergist appointment with my then 2 year old being scratched with a hypodermic needle (not kidding), then drops of allergy extract were dropped on the scratches, drops running from one scratch to the other, my two year old screaming in pain, he, I and his older sister forever traumatized. Even if this torture was okay, which it is not, how accurate was that test with extract dripping from scratch to scratch. I was so relieved when the blood tests became available.
Sounds horrific!
Thank you for sharing this. I had never considered any of it. I have had one skin prick test and was planning on doing more. I will not now. My daughter also wanted hers done…no. I’m excited that I think I know more now to make a better decision and just wanted to express my gratitude.
Thank you! xoxo
Gosh your article could not have come at a better time 🙂
I have been educating myself thoroughly on this subject and your recent post was perfect. Question: Can you still have an intolerance despite a test coming back negative? What is the difference between intolerance and allergy and aren’t vaccines also contributing to the rise in food allergies?
Hello Miss mama of three–I would encourage you to visit Dr. Joneja’s site for the most thorough information on intolerance vs. allergy. But basically, intolerances make you feel lousy while a true allergy involves the immune system and can potentially cause death. Yes, vaccines are playing a role, for the same immunological principles explained above. A good article on this is featured here: https://thinkingmomsrevolution.com/whats-really-behind-peanut-allergy-epidemic/ Thank you for reading! xoxo
Thank you so much for sharing this information which I will share with others! Recently someone close to me (an adult) was dealing with what appeared to be an allergic reaction — hives — and planned to see an allergist. It was just a very strong gut feeling I had to warn her to avoid skin tests. Fortunately, the doctor did a blood test instead. Thank you for confirming my gut instinct! God bless and take care…
Thank you for reading!
This…and the fact that the “allergy shots” so many of my contemporaries got when they were kids, contained a toxic amount of mercury.
Horrifying.
Rebecca, I had allergy shots for many years (born in the 60’s) and I had heard that they contained thimerosal – which makes sense as they were multi-dose vials. Do you know of any sources that show this? Thanks.
I’m commenting about a story about allergies posted 7 12 2018. Phenol look it on CDC website first. Now look up Hitler and phenol on wikipedia, please. Auto immune disease’s don’t exist! Causes (supposedly) Alzheimer’s, Parkinson’s, dementia, diabetes, lupus, impotence, eczema, psoriasis, arthritis, renal failure, anorexia, depression, suicidal thoughts, dehydration, starvation, constipation, MS,neuropathy, lupus, lymphoma, blindness, thoughts of killing people, PMS, schizophrenia, extreme fatigue extreme, addictive, thick toenails, hiv, asthma … 95% to 97% of all auto immune disease’s don’t exist! It’s a nerve blocker that was found in 1832! Nothing is hereditary. It’s all a lie. FBI has my records now. I have had a lot of these diseases. If you think that’s something it’s under different names and in just about everything including tires! Not a preservative, but slow money grubbing solution to screwing up your family! Jesus Walks
Maurice- there are phenols in a lot of foods that we eat that are good for us. I definitely believe that auto-immunity exists because the body can and does get confused via molecular mimicry and can attack self. I believe this to be have happened to my son. I believe the aluminum and glial cells helped to create a response to infection where the immune system is in overdrive this is overstimulating and leads to inflammation which contributes to seizures. He is being evaluated for post infectious autoimmune encephalopathy but I have been searching for help for years to figure this out and I am angry that I had to be a detective and that only a few brave doctors actually try outside of mainstream clinics. Autoimmunity is real. Yes phenol can be toxic but this is the phenol chemical. The phenols in foods can trigger responses and when my son was younger he was sensitive to phenols in foods and I blame the toxic load on that sensitivity. He can now handle phenols pretty regularly without the response. The flavanoids in phenol foods are important for health too. With all of the blue light that is around us I want him to have those colors in veggies and fruits. The plants have evolved with a protection that helps them and when we consume plants we utilize those protectants as we are complex microbial synergy. We must maintain a balance to sustain our life. Sometimes our illness is a healing crisis, sometimes our illness is a virus. My son likely has PANS and PANDAS (awaiting Cunningham panel) and what is interesting is I can literally witness these microbes and the cause and effect, sometimes a virus will cause inflammation and a seizure and then in the next couple days I see an improvement in symptoms from baseline and then the GAS molecular mimicry and the body go back to the extreme, it is as though this GAS hijacked my kid. I know about ASIA and I wanted Yehuda and Swedo to meet and discuss interventions so I did give Yehuda her info. I know that it might be a conflict of interest but I am sick and tired of these kids like mine, sick of no one giving a shit, sick of no one listening, and upset at the length of time and lack of awareness there is with autoimmunity.
I just want my kid back, if he has some autism ok but I want him to be more functional. I can say that diet does help, and I can say that sunshine helps but I need a stronger intervention because this extreme OCD gets in the way of life.
I believe that Diabetes, Asmtha and Allergies to function as an autoimmunity with everything else we are fighting.
Anyone try Patricia Kane Protocol with success?
Andrea, I totally understand where you are coming from. My son too has had a tragic story – from 10yrs old to now 18 but we are onto something now. Three things: We put him on a patch of Respen – A developed by Elain Delack RN – it is a homeopathic based on the radio frequency (resonance) of reserpine. My son could not speak intelligibly since he was 16 but within 3 months he is up to 4 words now repeating back to us and has stopped his gibberish for the most part. Each week is getting better. This is not a cure however but we want him to the point where we can understand each other so we can go to step 2 – Dr. Dewayne Smith has developed another radio frequency product he calls the “energy catalyst” which creates a condition of cleaning out the cell wall deficient pathogens (virus’, benzenes, phenols etc…) that gain access into the inner membrane of our mitochondria and block the cells energy production. It is extremely effective against lyme and cancer and I want to bring it to the ASD arena. 3. Parasites – this link is one that cannot be overlooked and will keep destroying the cell/nerves based on the continual production of ammonia (waste product of system parasite infestation) in the body that overwhelms our liver and kidneys etc… I bet you’ll notice the bad issues show up most beginning 3-4 days prior thru 3-4 days post the new and/or full moon. This is when parasites travel and reproduce within the body (colon to gut and back). I can be reached here – I just formed this group – you are welcome to join for more info. https://www.facebook.com/groups/397001440809390/?ref=bookmarks
Hi where are you finding help to diagnose pandas?
wow….. I had never heard that before, but I had known that most diseases were one in the same. I’m going to google phenol. That’s messed up!
Thank you for your comments.
Wow. I hope the tinfoil on your head doesn’t fall off, as you clearly need protection from the impulses the CIA is directing towards your brain. I suspect a few have gotten through.